The Positive and Calm Caesarean birth of Luka Anthony Williams
A thoughtful gift for new beginnings – buy a Calmbirth gift voucher

Story by Greer
Welcome Luka Anthony Williams, born Tuesday 31st May 2022.
Thank you Greer for sharing your amazing birth story!
Just so you have an idea, my husband Sam and I left Calmbirth feeling informed and empowered. We both had an understanding of each option available to us. Calmbirth helped facilitate discussion between us so we both understood our wishes and roles during labour and birth. We wanted to try and manage labour as naturally as possible. We hired a TENS machine and we were strongly against morphine and pethidine as pain relief options. We hoped to avoid induction, augmentation, epidural and caesarean if possible. We were open to monitoring, although I was keen to use the bath and shower so anything that restricted that was not likely to be ideal so we knew to ask about that. I was happy to have internal exams as necessary.
I was due to give birth on my birthday, June 4. At exactly 39 weeks, Saturday 28th May, I felt a little tired and decided to lay in bed about 4pm – something that I had hardly done throughout my pregnancy. I had some very mild period pain-like discomfort and thought that perhaps this was the start of something more.
I felt my first contraction late on the evening of the 28th. By 5am on Sunday 29th my contractions were 30-40 seconds long every 10 minutes, but this didn’t last long and things slowed down. Things were on and off between then and 2pm. I suspected my waters had broken but my midwife and the consultant obstetrician were happy for me to stay at home until contractions picked up again, which the midwife anticipated would happen as the evening came and my body relaxed into my night-time routine.
After a changeover of consultant obstetricians at the hospital, they decided they did want to see me to check where things were at. We arrived at the LGH about 5pm on the 29th. After an exam they were undecided if my waters had broken or not. Perhaps it had been a slow leak, but they decided that they hadn’t broken and I could go home again and wait for things to progress.
I was too uncomfortable to sleep Sunday night, although I tried my best to get some rest. Monday 30th May rolled around, which is my husband’s birthday. He was excited as baby had been due on my birthday but looked like he would be here on his! At 3:30am I had a much more significant gush of fluid and I was 100% certain my waters had broken. At 5am I had some bleeding and returned to the hospital again. They confirmed my waters had indeed broken this time and I was 2cm dilated, although my contractions weren’t close enough together to stay so we returned home at 7am.
By 10:30am I was struggling. My contractions were 4 minutes long. What we learnt in Calmbirth really came into play at this point. During each contraction I really couldn’t manage on my own, everything I had left in me was being spent on the contractions. I relied almost entirely on Sam to talk me through my breathing – he was such an amazing support. Every contraction he had to remind me – deep breath in… and out… Every. Single. Time. It was like my mind would go to another place and despite all my knowledge and practise I couldn’t implement calm breathing on my own. The TENS machine helped at some points, but at other points it wasn’t able to distract me from the feeling of the contractions. The breathing was probably the most helpful thing that got me through each contraction; both the breathing itself and the distraction of listening to Sam’s calm but direct instruction.
We rang the midwife and made our way to the hospital. I’d had severe swelling in my legs from 32 weeks and I was hopeful I could get in the bath in the birthing suite and I was lucky to have access to that. It was such a relief to get in the water. It meant I could kneel, which was something the swelling in my legs hadn’t allowed for so many weeks!
About 3pm the midwife said we should check and see how things were going. CTG showed baby was happy – his heart rate was 140bpm. Internal exam revealed that I was only 3cm dilated (but I was fully effaced). There was another lot of fluids that could be felt over baby’s head. We agreed to break these seeing as the clock was already ticking on the administration of antibiotics from when my waters had broken that morning. We were keen to get things moving to try and avoid antibiotics if we could. The midwife did a stretch and sweep at the same time which increased dilation to 3.5cm.
Intensity increased A LOT. 2 hours later I was exhausted. I felt like a zombie. I could barely tolerate the contractions and knew that I really didn’t have it in me to do any pushing anytime soon. Although we had been keen to avoid it, I asked for an epidural. Once the anaesthetist arrived it took 90 minutes and 4 attempts to get a successful epidural happening. I kept having different nerve pain through my hips and legs – I think it was just a challenge anatomically (the anaesthetist was fantastic).
Once the epidural was in… wow!! What an absolute relief. I realised how exhausted I was and it was almost a joy to be able to sink back into the bed and shut my eyes, even just for a moment. But it was still hard to sleep, I was so excited that our baby was soon going to be here. It also allowed me to be more present for the decision making that was about to come.
The obstetrician returned and along with our midwife discussed augmenting labour with Syntocinon given the length of my labour thus far and the lack of progression. I had been hesitant about induction and augmentation initially, but with the epidural going I was happy to progress with this. It had also been 18 hours since my waters had broken so they also wanted to start antibiotics for both my sake and baby’s.
Once all this was up and running we had some quiet time. Sam got some rest on the fold out chair, we both had a more substantial meal and we briefly remembered that it was still Sam’s birthday! Although given it was getting later into the evening it didn’t look like he was going to get a birthday buddy after all.
The last internal had been at 3pm and I was 3.5cm dilated then. I’d now had the Syntocinon drip in for approx. 3 hours at this point and it was a bit after midnight (I think… the timeline is a little fuzzy to be honest). The CTG had shown that baby’s heart rate had picked up to about 175bpm and increased every time they increased the Syntocinon dose. They wanted to check and see where things were at, which I was happy to do. I was only 4.5cm dilated.
The obstetrician returned and we talked through options. We could do a pin prick blood test from the top of baby’s head to check for lactic acid. If lactic acid was present then it would indicate that he was in distress. However, lactic acid would only be present if he had been distressed for 2 hours. So, if they tested and he had only been distressed for an 1.5 hours then it would probably come back negative. Alternatively, we could pursue an emergency caesarean. Of course, that came with its own risks. We only discussed it briefly.
The idea of our baby being distressed for any amount of time was not something we wanted, particularly when there was an alternative. We agreed to an emergency caesarean.
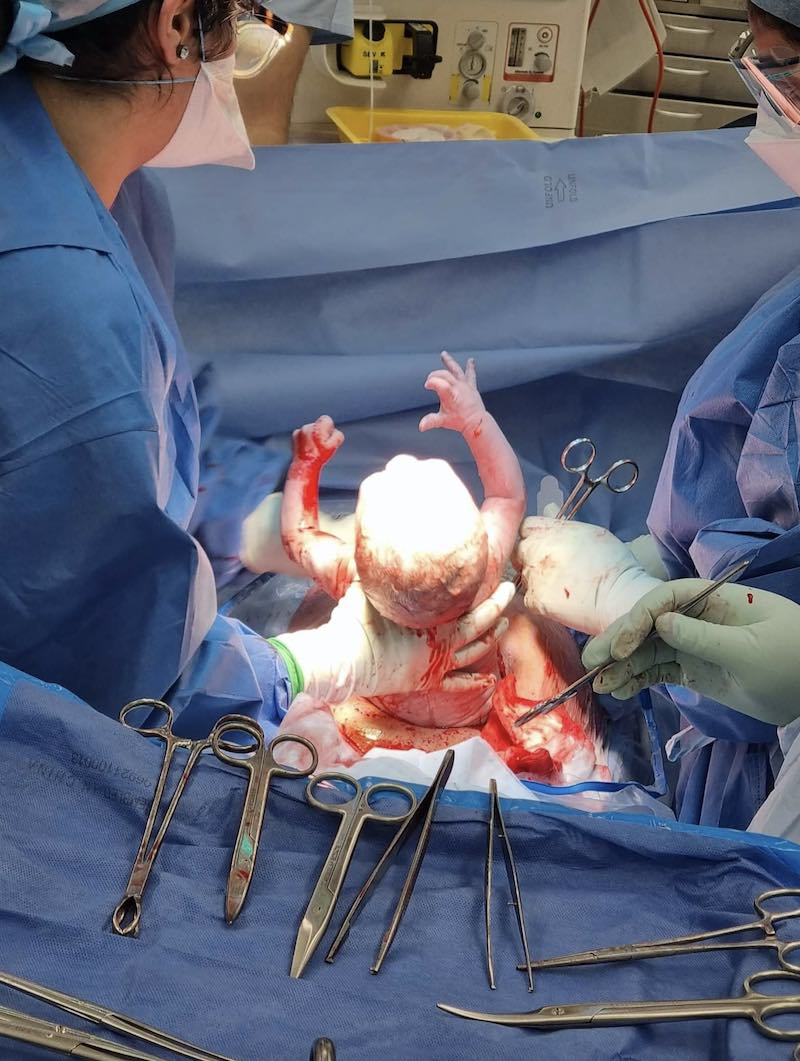
It was a whirlwind from there. People were coming and going, we were moved from the birthing suite to theatre. We met all the wonderful staff, including a fabulous anaesthetic nurse named Maddie who took nearly 200 beautiful photos of our time in theatre. Our baby boy Luka Anthony Williams came out screaming at 2:59am.
So, after having a strong preference for a natural labour and birth, we ended up having a birth that included antibiotics, epidural, Syntocinon and ended in caesarean. And it was absolutely perfect. We have a happy, healthy baby and I’m doing so well too. The obstetrician told us afterwards that Luka was both brow presentation and posterior. This accounts for why my contractions were so long early on (my uterus working overtime to try and get him into the right position in the birth canal when he physically wasn’t well positioned for such) and why I was taking so long to progress.
The LGH staff were all fantastic, through labour, birth, postnatally in the ward and once we returned home.
However, I think Calmbirth gave both Sam and I skills and knowledge that meant we could work harmoniously with the teams that looked after us. We had a bit of knowledge (nothing near what the staff have!) to be able to adequately discuss options and ask questions, but we also had a mindset that allowed us to tackle challenges as they arose. I can say that we truly did have a calm birth experience and I believe that’s having a flow on effect to our experience as new parents.
Thank you so much Cherie for your guidance through our Calmbirth experience. I would definitely recommend it to any expectant parents.



